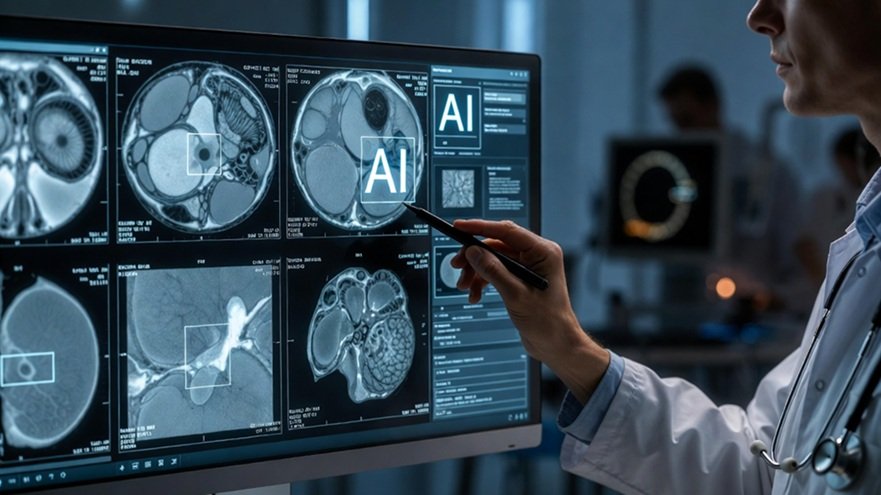
The Use of Artificial Intelligence in DICOM Medical Image Analysis
Share your love
 By: Dr. Elton Gómez, Specialist in Regenerative Medicine
By: Dr. Elton Gómez, Specialist in Regenerative Medicine
Contact: biohipercell@hotmail.com
Artificial Intelligence (AI) is transforming the analysis of medical images, particularly those stored under the DICOM standard (Digital Imaging and Communications in Medicine). This format not only contains the image itself but also critical metadata, including patient information, acquisition parameters, and clinical context. With the exponential growth in radiology studies, AI has emerged as a cognitive extension of the specialist, capable of detecting complex patterns, reducing interobserver variability, and accelerating clinical decision-making, opening new frontiers in personalized and regenerative medicine.
The DICOM standard represents a comprehensive ecosystem that combines image data in 2D, 3D, or 4D formats, structured metadata, and interoperability with PACS and hospital information systems. For AI algorithms, these metadata are not merely supplementary; they are essential for contextualizing each image and training robust models. By integrating clinical and technical information into a single analytical workflow, intelligent systems can generate more accurate and reliable results, improving the efficiency of medical processes.
AI approaches applied to DICOM analysis include classical machine learning, deep learning, and multimodal models. While traditional methods such as support vector machines or decision trees remain useful for smaller datasets, convolutional neural networks (CNNs) have transformed modern practice. These networks can automatically learn relevant image features, detect subtle patterns, and analyze full volumes from CT or MRI studies. Multimodal models combine imaging data with clinical information, prior reports, and molecular biomarkers, enabling predictive and integrative medicine.
 In clinical practice, these tools are already producing tangible results. In radiology, they support early cancer detection, automatic identification of fractures and hemorrhages, and prioritization of urgent studies. In neurology, they assist in lesion segmentation and volumetric brain analysis, while in cardiology, they optimize evaluation of ventricular function and detection of atherosclerotic plaques. In regenerative medicine, AI enables objective quantification of tissue regeneration, longitudinal study comparisons, and integration with molecular biomarkers, providing a more precise assessment of treatment outcomes.
In clinical practice, these tools are already producing tangible results. In radiology, they support early cancer detection, automatic identification of fractures and hemorrhages, and prioritization of urgent studies. In neurology, they assist in lesion segmentation and volumetric brain analysis, while in cardiology, they optimize evaluation of ventricular function and detection of atherosclerotic plaques. In regenerative medicine, AI enables objective quantification of tissue regeneration, longitudinal study comparisons, and integration with molecular biomarkers, providing a more precise assessment of treatment outcomes.
However, implementing AI in medicine faces technical, ethical, and regulatory challenges. Data quality and diversity are critical; population biases can lead to clinical errors. The need for interpretability has driven the development of Explainable Artificial Intelligence (XAI), which allows physicians to understand, validate, and supervise model decisions. Additionally, the privacy of DICOM data, traceability, and regulatory compliance are essential to ensure safety, trust, and institutional adoption.
Looking ahead, AI promises to become a real-time clinical co-pilot, integrating with augmented reality, assisted surgery, and regenerative medicine. Its true potential is realized when used ethically, regulated, and collaboratively with human judgment. Far from dehumanizing medicine, well-designed AI restores time, precision, and depth to clinical practice, enhancing the specialist’s ability to deliver more informed and personalized care.



